Trichoscopy in Trichotillomania: A New Diagnostic Tool
Online test
Find out the severity of your symptoms with this free online test
Trichotillomania (TTM) is a body-focused repetitive disorder characterized by repetitive hair pulling resulting in significant hair loss. It is estimated that the prevalence of trichotillomania is about 0.5% to 2.0% with symptoms often emerging in late childhood or early adolescence.
A diagnosis of TTM is based on clinical examination using the diagnostic criteria set forth in the Diagnostic and Statistical Manual of Mental Disorders 5 (DSM-5). Those criteria include:
- recurrent pulling out of one’s hair, resulting in hair loss
- repeated attempts to decrease or stop hair pulling
- the hair pulling causes clinically significant distress or impairment in social, occupational, or other important areas of functioning
- the hair pulling or hair loss is not attributable to another medical condition (e.g., a dermatological condition)
- the hair pulling is not better explained by the symptoms of another mental disorder
The diagnosis can be made by any qualified mental health or medical professional.
Making the diagnosis of TTM can be a challenge:
- Not everyone who presents with repetitive hair pulling meets the criteria for a TTM diagnosis and often only meet the criteria of recurrent hair pulling
- People are often unaware of the extent of their pulling, maybe in denial, or maybe hesitant to be open about their pulling behavior.
- Children, in particular, may be hesitant to admit that they pull their hair. Findings also show that about 50% of parents are unaware that their kids are pulling.
- TTM can present in ways similar to other dermatological conditions
If you’re like most people dealing with hair pulling and hair loss, your first stop might have been to your dermatologist’s office. While Trichotillomania (TTM) is considered a mental health disorder, dermatologists are often the first medical professional seen for issues related to hair loss.
Dermatologists use a number of tools to diagnose hair and scalp disorders. One tool in particular, trichoscopy, is widely used and has been suggested as a possible way to distinguish TTM from other dermatological conditions. Are there distinguishing signs of TTM under trichoscopy that can help to accurately diagnose TTM? A new study seeks to answer that question and explores the possibility of using trichoscopy as a diagnostic tool.
What Is Trichoscopy?
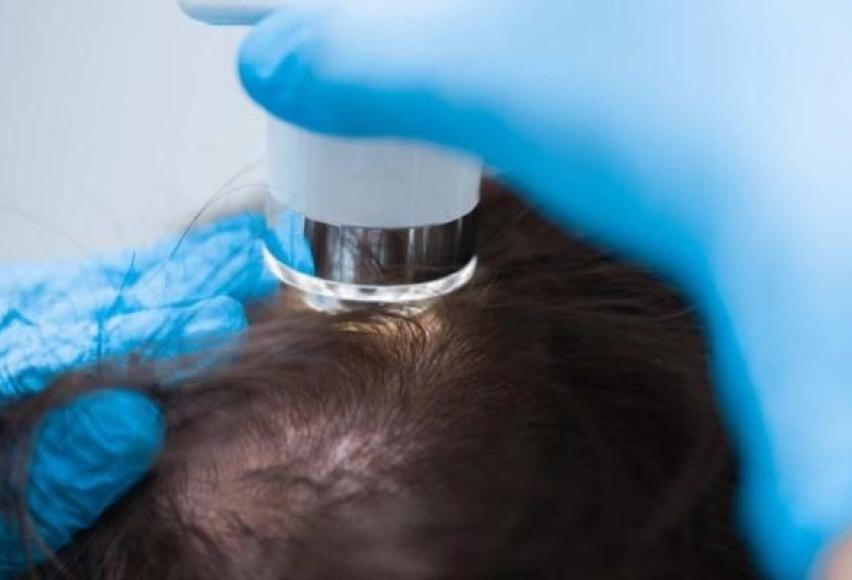
Trichoscopy is a term used to describe a dermoscopic evaluation of the hair and scalp, using either a handheld dermoscope or a videodermoscope. Trichoscopy lets dermatologists get a close-up view of what is happening at the surface of the scalp including the hair follicles. Trichoscopy is also used to evaluate treatment response.
Evaluation by trichoscopy is based on the close-up study of follicular patterns, interfollicular patterns, and hair signs. Trichoscopic patterns include:
- Follicular Patterns – white dots, yellow dots, black dots
- Interfollicular Patterns – pigment patterns, vascular patterns
- Hair shaft Characteristics – features seen in healthy vs. affected hair shafts such as shape, length, and other characteristics.
Within those patterns are specific features related to hair and scalp that can further identify specific skin disorders or inflammatory processes.
Being a mental health disorder, it would be reasonable to assume that pulling one’s hair in the absence of any disease process might not leave specific, tell-tale signs unique to TTM. However, it is a tool that dermatologists use quite frequently, and the condition of hair and scalp can yield important clues as to what’s happening. Studies have identified hair and scalp characteristics that would typically be observed in TTM and suggested that there may be some signs that are unique to TTM.
To date, there have been no large-scale studies examining what might be defining trichoscopy characteristics of TTM. This new study sought to broaden the understanding of trichoscopic characteristics and the role of trichoscopy inaccurate diagnosis of TTM.
Is Trichoscopy a Viable Diagnostic Tool?
This new study took what was previously known about trichoscopy and TTM a step further. Using data from a total of 13 previous studies, the data on trichoscopy findings were analyzed for sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV). It is important to remember that these signs are not easily observed without the use of trichoscopy.
The analysis revealed seven significant characteristics of TTM identified by trichoscopy:
- Trichoptilosis is the longitudinal splitting of hair shafts. While commonly found in people with long hair, for people with TTM, it is found in very short hairs in about 57% of cases.
- V-sign is a term used to describe when two or more hairs of a single hair follicle are pulled simultaneously and break at the same length above the scalp. The area is surrounded by longer, normal-length hairs. The V-sign is a characteristic of TTM with a specificity of about 99% and occurs in about 50% of people with TTM.
- Hook hairs or question mark hairs are hairs that are partially coiled. They are considered one of the most specific characteristics of TTM and were reported in about 43% of cases.
- Flame hairs are semitransparent, wavy hair residues that resemble a fire flame. They remain attached to the scalp after hairs called anagen hairs have been pulled. Anagen hairs are those hairs in an active growing phase. They were detected in an average of 37% of people with TTM.
- Coiled hairs are broken telogen/catagen hairs that curl back. Telogen and catagen hairs are more mature hairs. Coiled hairs were found to be highly specific to TTM and found in 36.8% of cases reviewed.
- Tulip hairs are short hairs with darker, tulip-shaped ends. These hairs are formed due to a diagonal fracture in the hair shaft. They were found to occur in 36.4% of the cases reviewed.
- Hair powder is a phenomenon that develops as a result of hair shaft damage that leaves a sprinkled hair residue remains. It is seen in TTM and sometimes in the forms of alopecia. It was found to be present in 36.4% of cases reviewed.
The most common characteristics found in people with TTM were broken hairs and black dots. Broken hairs were found in almost every case of TTM reviewed. However, their predictive value is low because they are also common in other hair and scalp issues. Black dots are pigmented residues of broken hairs on the scalp. They are not unique to TTM but are often observed.
The review also found that people with TTM tended to show a significant increase in capillary density and in hair growth which can be suggestive of TTM remission.
The Takeaway
The findings of this study suggest that trichoscopy is a viable and useful tool for the diagnosis and treatment of TTM. Several specific characteristics were identified that could help dermatologists more accurately distinguish TTM from other disorders that cause hair loss.
It also has the potential to be a useful tool for monitoring treatment response. Hair regrowth and scalp health can be observed. Being able to have this level of observational capability can reduce the risk of a patient’s lack of pulling awareness or reluctance to report pulling as complicating factors.
There is certainly more research to be done but trichoscopy offers dermatologists one more tool in their diagnostic toolbox. And, trichoscopy offers help and hope to people living with TTM and other hair and scalp disorders. A correct diagnosis is the foundation of effective treatment.
References
1. Grant, J. E., & Chamberlain, S. R. (2016). Trichotillomania. The American journal of psychiatry, 173(9), 868–874. https://doi.org/10.1176/appi.ajp.2016.15111432
2. Rudnicka, L., Olszewska, M., & Rakowska, A. (2012). Atlas of Trichoscopy: Dermoscopy in hair and scalp disease. Springer Science & Business Media. https://books.google.com/books/about/Atlas_of_Trichoscopy.html?id=oNdm2o19jG0C
3. Chandran, N. S., Novak, J., Iorizzo, M., Grimalt, R., & Oranje, A. P. (2015). Trichotillomania in Children. Skin appendage disorders, 1(1), 18–24. https://doi.org/10.1159/000371809
4. Kaczorowska, A., Rudnicka, L., Stefanato, C. M., Waskiel-Burnat, A., Warszawik-Hendzel, O., Olszewska, M., & Rakowska, A. (2021). Diagnostic Accuracy of Trichoscopy in Trichotillomania: A Systematic Review. Acta dermato-venereologica, 101(10), adv00565. https://doi.org/10.2340/00015555-3859
5. Jain, N., Doshi, B., & Khopkar, U. (2013). Trichoscopy in alopecias: diagnosis simplified. International journal of trichology, 5(4), 170–178. https://doi.org/10.4103/0974-7753.130385
6. Yorulmaz, A., Artuz, F., & Erden, O. (2014). A case of trichotillomania with recently defined trichoscopic findings. International journal of trichology, 6(2), 77–79. https://doi.org/10.4103/0974-7753.138597
Online test
Find out the severity of your symptoms with this free online test
Start your journey with TrichStop
Take control of your life and find freedom from hair pulling through professional therapy and evidence-based behavioral techniques.
Start Now



