Trichotillomania Diagnosis and the DSM5
Online test
Find out the severity of your symptoms with this free online test
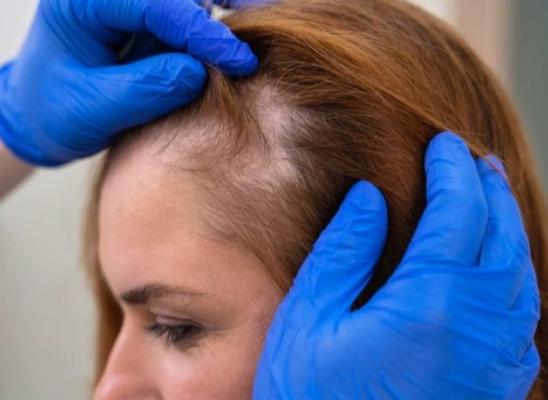
It is not uncommon for people to subconsciously play with, twirl or pull at their hair when anxious, tired or bored, nor is it uncommon for people to routinely pull out grey hairs or split ends. For many repetitive hair pulling is just a bad habit that has no real impact on their daily lives. But for some, this practice can be so consuming that it starts to have a negative impact on day to day functioning, their social lives, and can cause significant emotional distress. In these instances, hair pulling has evolved from a bad habit into a recognized clinical disorder known as trichotillomania, or compulsive hair pulling disorder. Because of the poor awareness by the general public that such a disorder even exists, hair trichotillomania often goes undiagnosed and therefore untreated, with many sufferers suffering in silence for many years.
How will I know if I have hair pulling disorder?
There is such a fine line between hair pulling as a bad habit and the onset of a clinical diagnosis that is is often shrugged off and dismissed by those affected by it, as well as by health professionals who are not knowledgable about trichotillomania, and perceived as a habit the person simply needs to 'get over'. Yet when the behviour has escalated to the level of a diagnosis, this is exactly what they struggle with most. One of the key clues that behaviour may have a clinical component is if the individual has tried to stop pulling on several occassions and failed, often leading to the beaviour actually increasing as a result. Some of the warning signs that hair pulling is affecting your function include:
- Not being able to go out in public without covering up the pulling site, e.g. wearing hats, scarves, sunglasses
- Avoidance of social situations when conditions are windy or wet, e.g. swimming
- Constantly being late due to spending extended periods of time pulling
- Feeling you are not in control of the ability to stop pulling

Classification and the DSM
In a previous article on this site we outlined the history of trichotillomania classification in the Diagnostic and Statistical Manual (DSM) of the American Psychiatric Association. Trichotillomania was only first recognized in the DSM-III Revised edition (DSM-III-R) in 1987. Since then the diagnostic criteria have been revised to the current version found in the DSM-5. The DSM-5 clearly differentiates hair pulling as a disorder from other non-clinical hair pulling behaviours. For example it states that “Trichotillomania should not be diagnosed when hair removal is performed solely for cosmetic purposes”. The DSM-5 also recognizes the diversity of the disorder, so one cannot determine whether you have trichotillomania solely by comparison to others who have the disorder. The DSM-5 characterizes trichotillomania by recurrent repetitive behaviour (hair pulling) and repeated attempts to decrease or stop the behaviour. The behaviour can occur during both relaxed and stressful times, but there is often a mounting sense of tension before hair pulling occurs or when attempts are made to resist the behaviour. Trichotillomania is categorized under obsessive-compulsive and related disorders (OCRD) and the criteria for diagnosis are as follows:
- Recurrent hair pulling or plucking resulting in visible hair loss
- Repeated attempts to decrease or stop hair pulling
- The hair pulling causes clinically significant distress or impairment in social, occupation, or other important areas of functioning
- The hair pulling is not attributable to the psychological effects of a substance (e.g., cocaine) or another medical condition (e.g., scabies)
- The hair pulling is not better explained by symptoms of another mental disorder (e.g., delusions or tactile hallucinations in a psychotic disorder, attempts to improve a perceived defect or flaw in appearance in body-dysmorphic disorder, stereotypes in stereotypic movement disorder, or intention to harm oneself in non-suicidal self-injury)
The inclusion of trichotillomania as well as excoriation (skin picking) disorder in the DSM5 indicate huge progress in the awareness and understanding of the condition. However there is still a long way to go with a working group being tasked to make recommendations for the classification of these conditions in the eleventh edition of the International Classification of Disease (ICD-11), which is the global classification of disease endorsed by the World Health Organization (WHO). A recently published report by members of the working group recommended that consideration be made for the classification of trichotillomania and excoriation disorder in a unique category of body-focussed repetitive behaviors (BFRBs) along with the other BFRBs in both the ICD and the DSM, whilst maintaining the definition presently used in the DSM5. This is because it is widely accepted that trichotillomania and skin picking disorder most closely resembles characteristics of the other BFRBs. Currently trichotillomania and excoriation disorder are categorized under obsessive compulsive and related disorders, while body-focussed repetitive behaviours such as onychphagia are categorized under "Other Specified and Unspecified Obsessive-Compulsive and Related Disorders"
Awareness is Key!
What is clear is that there are definitive guidelines for the diagnosis of these conditions and that health professionals should be educated to identify the signs and symptoms in their patients, and the stigma attached to these behaviors need to be addressed to ensure that more people are diagnosed sooner and receive the help they need.
Online test
Find out the severity of your symptoms with this free online test
Start your journey with TrichStop
Take control of your life and find freedom from hair pulling through professional therapy and evidence-based behavioral techniques.
Start Now